Is Medtronic’s MiniMed 640G an Artificial Pancreas?
Commentary
People with Type 1 diabetes may have felt a flutter in their hearts when they saw headlines that a 4-year old boy from Australia was fitted with a new type of diabetes pump technology. That’s because some news outlets, including the Guardian (UK) and the West Australian, labeled the new device an “artificial pancreas.”
By employing those two magic words these two news outlets waded into a debate that has been simmering behind the scenes in the diabetes community for several years: what exactly is an artificial pancreas?
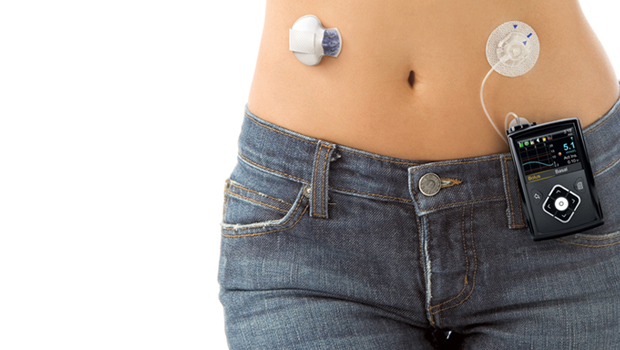
The device in question is the new Medtronic MiniMed 640G, which uses improved algorithms and an integrated pump-and-continuous glucose monitor system to anticipate blood sugar levels and suspend insulin delivery if those levels are trending downward. The system is being rolled out on a global scale by Medtronic this month, but is not yet approved in the U.S. By predicting blood sugar levels, the pump is a step up from Medtronic’s 530G pump, which can only shut off insulin delivery when it senses a low blood sugar level. The 640G seems to be a great answer to nighttime hypoglycemia and “dead in bed” syndrome. A pump that can anticipate blood glucose levels is sometimes also called a bionic pancreas.
For some, this innovation is good enough for the pump to earn the title of artificial pancreas, but it’s important to note that even Medtronic stopped short of calling it that. The press release sent to news editors suggested that the device was “Another Step Towards an Artificial Pancreas”. Medtronic suffered significant public relations fallout from the diabetes community when its promotional material for the 530G failed to make such a distinction.
Many other news outlets were more careful than the Guardian on the 640G. The Australian Broadcasting Corporation labels the new device a “world-first insulin pump”, while the New York Times newsfeed labeled it a “pancreas-like device.” Such convoluted phrasing comes about because there are many in the diabetes community who believe a true artificial pancreas must do two things: predict blood sugar level trends and provide glucagon to bring blood sugar levels back up when they go too low. The idea is to create a nearly-closed-loop system with minimal user input; no longer would it be necessary to eat or drink to correct for lows.
 There are even a few in the diabetes community who would not consider a dual-hormone pump an artificial pancreas. The argument is that the natural pancreas actually regulates several different hormones, not just glucagon and insulin, and all the pancreatic hormones are necessary to maintain normal blood glucose levels.
There are even a few in the diabetes community who would not consider a dual-hormone pump an artificial pancreas. The argument is that the natural pancreas actually regulates several different hormones, not just glucagon and insulin, and all the pancreatic hormones are necessary to maintain normal blood glucose levels.
This kind of labeling confusion can create an emotional roller coaster for those with Type 1 diabetes or who care for children with Type 1 diabetes when they read headlines about a new predictive pump. That being said, you would be hard-pressed to find someone in the diabetes community who isn’t excited about advancements like the MiniMed 640G, no matter what it is called. Predictive pump technology is another important step on the journey to nearly-hands-free daily care for Type 1 diabetes.
Now comes the hard part: waiting for the MiniMed 640G to reach U.S. shores. It’s anticipated that Medtronic will seek FDA approval for the 640G sometime in 2015.
Thanks for reading this Insulin Nation article. Want more Type 1 news? Subscribe here.
Have Type 2 diabetes or know someone who does? Try Type 2 Nation, our sister publication.







