Inside The Bionic Pancreas Inpatient Trials

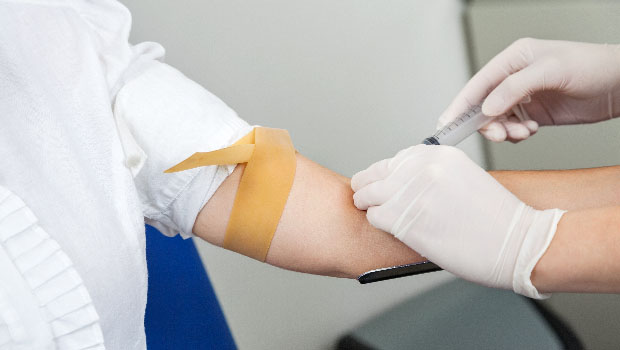
1 Cathy Grzesik (52) during her tests,
2 Emily Burke (16) eating a high-carb dinner,
3 Dr. Steven Russell with Emily’s Dad, Pat, reviewing Emily’s data on Dr. Russel’s cell phone and
4 Dr. Steven Russel.
There is an old saw that luck is what happens when preparation meets opportunity, and Ed Damiano’s relationship with Dr. Steven Russell is a perfect example of the saying in action. In 2006, when Damiano came to the Joslin Diabetes Center to give a talk about the experiments he was doing on pigs, using an early version of the bionic pancreas. Russell happened to be in the audience.
Russell recalls, ”After Ed finished, I approached him and told him that he should be testing this on people, and that I wanted to help.” Russell, an endocrinologist who does basic science research at Joslin, is also on the staff of Massachusetts General Hospital. Damiano and Russell are still working together, moving deliberately and inexorably toward a broad clinical trial of their closed-loop system.
The most recent trial, which Insulin Nation was allowed to record, focused on 24 different type 1 PWD, 12 years and older, all of them pumpers. In general, the trials test how the control algorithm responds to and how effectively it manages each individual’s diabetes over a 48-hour period during which the device assumes total control of both insulin and glucagon doses.
This particular group is divided in two, for research purposes. Twelve subjects receive a priming bolus of insulin at the beginning of each meal that automatically adapts to the PWD’s insulin needs based on what the system learned from previous meals. In the other twelve subjects, the system is entirely reactive, and no priming bolus is given. Although the next version of the bionic pancreas will allow each wearer to tell the system whether they are eating a small, medium, or large meal (the groups are based on carbohydrate ranges), in this test all of the meals are large, ranging from 80 to 120 grams of carbs each. In addition to eating meals that will push the system to respond to higher levels of glucose, each subject also spends 30 minutes on an exercise bike, pedaling at a moderate pace, so that the system has to prevent hypoglycemia by using glucagon. Each subject’s glucose level is measured both by a CGM similar to the one that will be in the final product, and by a hospital glucometer connected to an IV. The control system only gets the CGM measurements, but the measurements from the IV allow the team to know how well the system did in controlling the true BG regardless of how accurate the CGM was.
On a subject’s first day, the system assumes control precisely at 3 p.m. Damiano usually visits each person between 4:30 and 6 p.m. Before he enters the subject’s room, he pauses in the hallway to assemble the wearable prototype, slipping his iPhone into a slightly larger and thicker case that is a replica of the final product. Then, with the magic act in his pocket, he introduces himself, explains the meanings of the readings on the screen of the Apple laptop connected to the subject, and finally, shows the prototype. His standard attire of dark t-shirt, jeans, and running shoes may seem a bit unusual in the hospital environment, but the subjects don’t seem to care. They see him with the hope that maybe, just maybe, they can live with diabetes without it being the center of their existence.
Thanks for reading this Insulin Nation article. Want more Type 1 news? Subscribe here.
Have Type 2 diabetes or know someone who does? Try Type 2 Nation, our sister publication.