We’ve Tried Everything for My Daughter’s Insulin Allergy
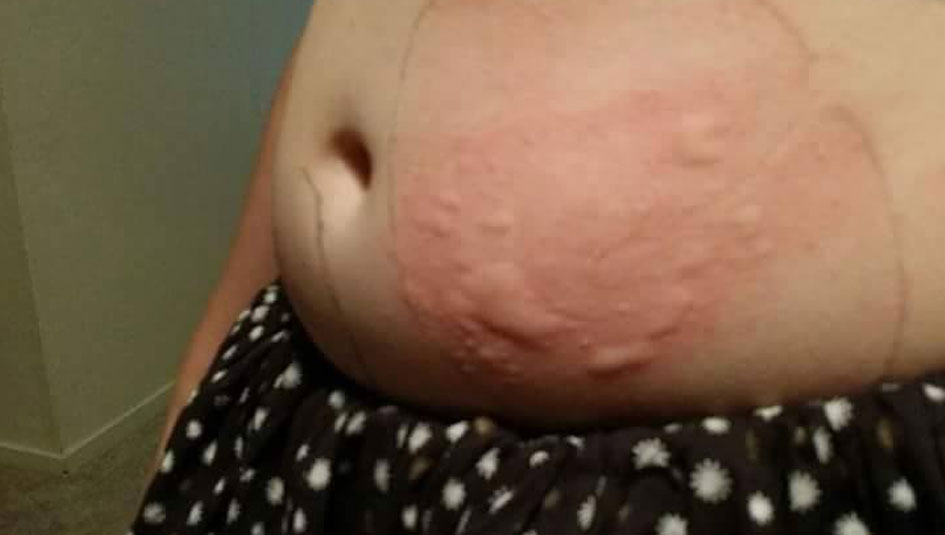
My daughter was diagnosed with Type 1 diabetes at the age of four, right when her blood sugar began to rise. We were fortunate to catch it early, for if it had progressed to when she would have needed an IV drip of insulin, the medicine itself might have killed her.
After being in the hospital for three days after that diagnosis, we were cleared for Emmy to go home. The caveat was that we had to show the nurses that we could give her a shot. It was decided to send her home on half a unit of Lantus. My husband gave the shot and we walked out the door.
Read “I’ve had an insulin allergy for 33 years.”
On our drive home, though, Emmy began to itch, a lot. At home we noticed a red spot, so we called our endocrinologist. He said to watch it. A few hours later, Emmy came down the hall stumbling and grabbing her throat. She could barely breathe. We called 911. After a night in the ER with an IV of antihistamines and steroids, we were allowed to go home again.
Early in the morning, Emmy began to wheeze again, and this led to an early morning visit with our endocrinologist. Everyone felt it was the insulin, but it was strange to have this kind of reaction happen. She was switched to Levemir and we gave the shot at the office. She didn’t get a red spot and we thought we were in the clear.
Read “Insulin Allergies are for real.”
A few weeks later, the honeymoon waned and she needed to start on fast-acting insulin. She was put on Apidra and again developed a red spot, only quicker this time. The itching came, too. We began to give lots and lots of antihistamines. After her reaction settled, it was agreed by all the doctors that she was also allergic to Apidra. So we tried Humalog – no red spots. At this point, everyone was only cautiously optimistic.
We were notified by Sanofi-Aventis that the only ingredient that was different between Humalog and the other insulins was Polysorbate-20. That meant our daughter must have been allergic to this chemical.
Over the next year, we called and saw many doctors. We wanted to know if there was anything we could do. After all, two of the six insulins stopped her breathing – what if she couldn’t tolerate the other four? No one could or wanted to do any testing. It was too dangerous, they said, and she was “not allergic to the other insulins.”
Over the next year, Emmy’s skin began to show marks; touch brought raised redness. She was diagnosed with dermatographia, a skin condition where one can literally write their names on their skin with a finger. We talked with the head of Cedar Sinai Immunology. He said chemical allergies were hard to treat and that trying to desensitize her could kill her. Since she was tolerating the other insulins, we were told to just be diligent and keep polysorbate out of the house. We asked about testing – we wanted to be sure it was the polysorbate – and were told that it couldn’t be done.
A year into her diabetes, Emmy got a pump because her diabetes was so hard to control. Her blood sugar levels would suddenly jump and drop for no reasons. Her endocrinologist was confused.
Pump use brought pump failure. Her whole side of her body broke out in hives. We tried to move her back to shots, but she would get welts and hurt so much she would vomit. This is when it was decided that she must be allergic to the Levemir and Humalog. We put her on Benadryl and Novolog. Over several years, local doctors tried many variations of OTC and prescription allergy and antihistamines. They tested her against all the common and uncommon allergens. She was allergic to none.
We got her seen at Stanford University. The doctors who examined her there felt that she was reacting to meta-Cresol, an organic compound in the insulins. Again we asked for testing to confirm this and were told it wasn’t possible. For over a year, doctors with the Lucile Packard hospital at Stanford tried to get the chemicals we needed so we could attempt inpatient desensitization, with no success.
We reached out to a doctor in New Zealand, who was the only doctor up to this point who had successfully treated this allergy. He gave many suggestions. We pushed Stanford to do something. They decided to try Immunosuppressive Therapy along with high doses of prednisone and a low-carb diet. Emmy had to be kept at home or wear a mask when she left the house, but for the first time in years, she didn’t hurt and her blood sugars were steady.
We tried to lower the prednisone but couldn’t get below 10 mg a day without reactions. Then her creatinine levels began to rise and they were worried that she would have kidney damage if we continued. The immunosuppressive therapy was stopped, but not the prednisone. Then Emmy developed cellulitis and they were worried it had gone into the blood. It was agreed to stop the prednisone. Her reactions came back.
Stanford decided to try several other therapies, including adding steroids into her insulin so that it was only at the site. Nothing worked. We decided to transfer to UCSF. They immediately increased her allergy and antihistamines doses and wanted to do more tests, but needed the meta-Cresol. They tried for over a year, and only were able to obtain a tiny amount on the week we were scheduled to relocate to South Carolina. We were only able to get one test done, the one they didn’t think would show anything but was the least risk.
Within days of our relocation, we got Emmy established at the Medical University of South Carolina. At our first visit we were told that they were not sure how much they could do, aside from minimizing the symptoms. Our new immunologist told us that it comes down to access to the test kits and chemicals.
Doctors don’t know for 100% certain that she is allergic to both the polysorbate and meta-Cresol. The diagnosis is one of “everything else is removed, so therefore it must be…” If we could test, then we could possibly petition for insulin without these ingredients.
Emmy cannot tolerate any long-acting insulin. She describes shots of short-acting Novolog this way: “Well, it’s a deep burning…that turns into a fire that sort of spreads through my whole body.”
 Most recently, a gastrointestinal doctor diagnosed her with functional abdominal pain syndrome. It is believed to be due to all the histamine in her body because of her reactions to insulin. He wants to add periactin, a powerful antihistamine, to her regimen, but this would mean that she would be even more sedated and only awake a few hours a day.
Most recently, a gastrointestinal doctor diagnosed her with functional abdominal pain syndrome. It is believed to be due to all the histamine in her body because of her reactions to insulin. He wants to add periactin, a powerful antihistamine, to her regimen, but this would mean that she would be even more sedated and only awake a few hours a day.
After 8 years, my daughter now daily takes:
Novolog
Xyzal- (5 mg, antihistamine)
As needed, she also takes:
Atarax (25 mg – antihistamine)
Benedryl (50 mg – antihistamine)
Zofran (8mg – for vomiting)
EpiPen (for when the reaction is really bad)
Ibuprofen
She is almost 12 years old and this is her life. My daughter doesn’t wish for a cure for diabetes. Her wish is to be like all the other people with Type 1 and be able to take her insulin without feeling immense pain or violently ill.
If you are a medical researcher who would like to contact Tiffanie about her daughter’s case, please email our editor at cidlebrook@epscomm.com.
Thanks for reading this Insulin Nation article. Want more Type 1 news? Subscribe here.
Have Type 2 diabetes or know someone who does? Try Type 2 Nation, our sister publication.







