A Shot From the Past

Itʼs easy to take diabetes technology for granted and be displeased with any medical gadget that is not ultra-convenient, accurate to an inch of its life, and possessed of certain chic design elements. Having had Type 1 diabetes for decades, however, I know just how far we’ve come.
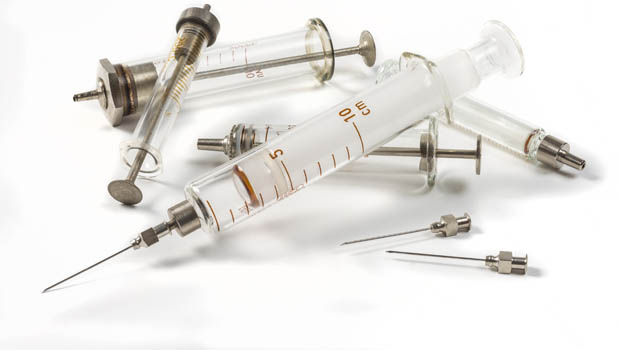
I was diagnosed in 1969 at the tender age of 16 months. In those days, you had many fewer options for insulin. You injected a long-acting insulin once a day, and it was probably lucky it was only once since it was quite a procedure. You had to boil up glass syringes and resharpen needles over a hotplate to sterilize them.
The Childrenʼs Hospital had sold us an automatic injection device that looks positively gruesome by todayʼs standards. You placed the glass syringe with the detachable needle into the gun, put it in position, clicked the lever, and the needle was propelled into you. Mum used it on me when I was younger, but I could never bring myself to do it until I was about 8 years old. By then, plastic hypodermics had become available.
There was no such thing as home blood glucose monitoring, either. To get some vague idea of what your sugar had been doing in the last 10 hours, you had to go through a complicated process of collecting your urine and then using an eyedropper to mix 5 drops of urine and 10 drops of water (or was it vice versa? I really canʼt remember now) in a test tube. You added a tablet which produced a frothing mixture that would now seem more at home in a Harry Potter class. You then compared the resultant color to a handy little color chart; blue meant “negative” or no sugar present, and orange was more than 2% sugar. Of course at the time of testing, you might show “orange” but really be experiencing hypoglycemia because your urine reflected the past, not what was happening now.
(Testing for ketones was slightly easier. You just had to put urine on a tablet and if the tablet turned purple, then you were in trouble.)

In 1979, I got to witness probably the single biggest technological improvement care in my childhood when the Sydney Childrenʼs Hospital began to put its Type 1 patients onto home blood glucose monitoring. This came about because of one diabetes dad’s tinkering. Stan Clarke was an engineer and his daughter was a Type 1 patient at the hospital. He went to his garage one day in 1978 and made an inexpensive home glucometer, called simply the “machine” by hospital staff.
The machine was the size of a brick. You calibrated it with a screwdriver and it had a needle and dial for readings rather than spitting out exact numbers, but it changed my diabetes life. At long last there was some certainty! With the machine and the advent of better insulin, we finally possessed some ability to actually do something when our blood sugar levels were too high.
Of course there was no such thing as lancets, let alone lancing devices available for purchase then. In an affront to asepsis everywhere, I used to just jab my finger with a preloved hypodermic. I never did get an infected finger. (Warning: This is bad. Donʼt try this at home, folks).
Now I have a glucometer that sends my blood sugar levels to my pump and calculates a correction bolus if required. I can give insulin doses to one-tenth of a unit with the push of a button. At the end of the day, these tools have changed my life, and diabetes management is cleaner and has at least the veneer of greater accuracy. It’s still up to me to take charge of my Type 1 diabetes, however, and that hasn’t changed since the seventies.
You can read more from Melinda Seed at her blog http://twicediabetes.com/.
Thanks for reading this Insulin Nation article. Want more Type 1 news? Subscribe here.
Have Type 2 diabetes or know someone who does? Try Type 2 Nation, our sister publication.







