Living with Type 1 Diabetes in 1959
“Having diabetes nowadays isn’t easy, but in 1959 it was hell,” says Debbi Tally, who was diagnosed with T1D at the age of 8 years old
Doctors told Debbi’s parents she wouldn’t live to be 14 years old.
Her friends and teachers thought type 1 diabetes was contagious, so she wasn’t allowed to play with other children and many teachers didn’t want her in their classroom.

My high school principal said I couldn’t go on the senior class trip because I was a danger to other children because of my diabetes.”
Debbi is now 69 years old. The doctors were very wrong — about a number of things.
Unable to check blood sugar levels
For the first several decades of Debbi’s life with type 1 diabetes, she was essentially unable to ever actually check her blood sugar levels.
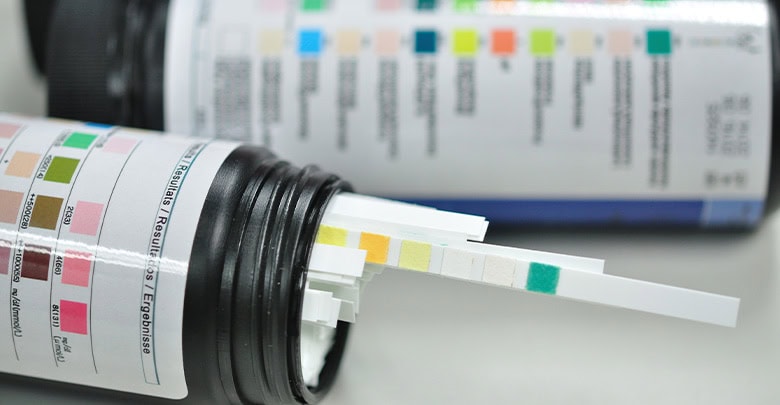
“Back in those days, the only way to check your glucose levels was by using a urine test strip. The problem was that the results it gave you were from two hours ago, and they were a range, not a specific number,” explains Debbi.
In other words, the methods available for checking your blood sugar were essentially useless.
Instead, Debbi took insulin NPH and Regular insulin and juggled her blood sugar levels by feeling the symptoms and inevitably experiencing a lot of low blood sugars.
A testament to just how often Debbi struggled with low blood sugars was evident in her HbA1c, which was often as low as 4.9 percent.
Back then, low blood sugars were called ‘insulin reactions’,” explains Debbi. “My mother would get mad at me because she thought I had done something purposefully to mess things up.”
Severe hypoglycemia and seizures became very common for Debbi. Her mother would inject glucagon and call an ambulance at least once a month. The seizures became so frequent that Debbi was eventually misdiagnosed as also having epilepsy.
“The doctors started making me take Dilantin — an epilepsy drug for seizures. But my seizures kept happening,” says Debbi, recalling the frustration. “After going to diabetes camp for the first time and watching other kids have seizures because of low blood sugars, I was sure I didn’t have epilepsy.”
Worse, Debbi felt the epilepsy drugs she’d be forced to take were actually causing further seizures since she wasn’t actually epileptic.
“I finally convinced a neurologist that I didn’t have epilepsy. He admitted that he was just following other doctors’ notes and finally did his own tests.”
Fortunately, he concluded that Debbi didn’t have epilepsy either and took her off the meds, which immediately reduced the frequency of her seizures!
Using the same syringe for years
“We used the same needle for two or three years, basically until it broke,” Debbi recalls. “They just didn’t believe in changing it.”
Debbi’s syringe was kept in a mason jar that also contained cotton balls and rubbing alcohol to keep it sterile. After each injection, it would also be dipped in boiling water.
When the needle wouldn’t puncture my skin on my thigh, that meant my mother had to remove the burrs that had built up, making it too blunt.”
Debbi and her mother would remove the burrs (which aren’t really visible to the naked eye) by taking a pumice stone to the needle to essentially re-sharpen it.
Transitioning to newer technology in 1985
“I was the first employee at my work to have an insulin pump, but in order to get a pump my doctor said I had to start checking my blood sugar more often,” recalls Debbi.
Having never been able to accurately check her blood sugar for the prior 20 years of her life with type 1 diabetes, Debbi had little understanding of just how useful these newer blood glucose strips and meters would be to her.
“I was vaguely aware of it but I didn’t understand the purpose of it because I’d lived with type 1 for so long without ever being able to check my blood sugar. My A1c was fine and I went to my regular doctor appointments, I didn’t think I needed or had time to check my blood sugar.”
Motivated by the idea of using an insulin pump, Debbi started using a glucose meter, too.
“I started seeing just how much my blood sugars were truly fluctuating. It was very eye-opening.”
She asked her healthcare team for a prescription to get more test-strips in order to keep up with her very active job as a police officer and eventually working for a security team.
Eventually, Debbi was asked by her healthcare team to be part of a team that would help other patients learn how to treat their diabetes. While there was little-to-no diabetes education available in the 60s and 70s, the newer technology meant more information which led to more opportunities for education.
Thriving today against the odds
Despite living with type 1 diabetes for decades when technology and insulin were minimal, Debbi is 69 years old today with no diabetes complications.
Debbi has a 47-year old daughter despite being told she would never have children.

She thrived in a career as a police officer and security guard. And watch out, because she was the second-best shot (with her pistol) out of all the officers in her county during her police career.
Debbi was diagnosed with Celiac disease at 50 years old but has used it as merely another motivation to make healthy decisions for her daily life.
With 50 years of type 1 diabetes under her belt, Debbi has spent years helping educate and encourage other patients through health fair events and support groups.
Accolades for Debbi Tally include:
- Diabetes On Target Groups 607-776-4065
- Founder, President, Diabetes Educator & Diabetes Advocate
- 50 Year Joslin and Eli Lilly Medalist
- 2013 Jefferson Award
- Bath Rotarian
- 2016 Paul Harris Award