The Doctor is (Always) In
Diabetes has always been a lonely disease. Unlike other dangerous maladies, such as cancer, it tends to isolate those who have it, drawing them into themselves rather than connecting them to a circle of medical help, family support, and encouragement. When we talk about someone’s diabetes getting attention from others, we often call the would-be helpers the “diabetes police.” These cops aren’t helping us cross the street—they’re nagging us to death. The cherry on top of this sundae is the quarterly or semiannual doctor’s visit, at which many of us are reminded that our numbers show we aren’t doing what we’ve been told.The caregivers are frustrated too. Most doctors and other medical professionals want to help people stay well or get better, and often the results show that isn’t happening. Part of the problem lies in trying to fit diabetes into the normal routines of medical care, which combine periodic office visits with acute situation response. There isn’t any room in this scenario for a condition that requires everyday care outside of an institutional setting. If it takes a village to raise a child, it takes a team to control diabetes, and the situations that arise can’t or shouldn’t wait 90 or 180 days for treatment.

It can be a vast circle of frustration, but different approaches that empower both sides of the care equation are emerging. Some call them “connected care,” others refer to “telehealth.” Whatever the label, connected care removes the loneliness from diabetes care by using “smart” devices to share information with others. More than 30 years after the first personal glucometers were introduced, today’s technology innovations enable a team approach to treatment, and allow both patients and caregivers to act on new, more nuanced, information immediately.
Telcare – Insight From The Cloud
For a snapshot of connected care’s benefits, let’s examine the case of Steve Powered a middle-aged man in the Piedmont area of North Carolina with Type 2 diabetes. He is one of up to 5,000 people with chronic conditions like diabetes who receive medical care from Carolina Advanced Health Care (CHA), a joint venture between Blue Cross Blue Shield of North Carolina and the University of North Carolina at Chapel Hill. A central feature of the practice is its commitment to telemonitoring of diabetes; there are two dedicated “telehealth” rooms on the premises.
Some Carolina Advanced Health Care diabetes patients, including Steve, use a glucose monitor made by Telcare (www.Telcare.com), a privately owned diabetes technology company headquartered in Maryland. The Telcare meter is also a cellular device that automatically uploads every test result into a Cloud-based data warehouse. There the results are organized into a series of charts and graphs, which can be viewed by the patient or anyone he chooses, including his or her medical team and family members.
In Steve’s case, Dr. Thomas Warcup, a family practitioner who also is the head of Carolina Advanced Health Care, was one of the medical professionals looking at his data. “We noticed that his fasting blood glucose levels were reasonable,” Warcup said,” but his numbers spiked every day after he ate lunch.” Armed with that information, a nutritionist on CAH’s staff, who had already met with Steve, called him and asked what he was eating. Steve changed his food choices and the midday, his numbers dropped dramatically. “If I can get them [patients] to understand the impact that lifestyle choices have on blood sugar” Warcup said, “we can make real progress. I think giving people specific examples in real time based on our observations of their data is powerful. Neither of us should have to wait 90 days or six months to talk about this.”
WellDoc – Prescription Apps
Another young company that embraces mobile health and real-time intervention is WellDoc (www.welldoc.com), also based in Maryland. Founded in 2005 by an endocrinologist who was frustrated because she couldn’t adequately support her patients between office visits, the company has developed a prescription-based platform that is part of a new category of Mobile Integrated Therapies, or MIT. Scheduled for a full rollout in mid-2013, WellDoc equips physicians with the tools to offer a form of personalized medicine and real-time coaching through any data-enabled device. The key is patient data (lifestyle, medication, glucose, or symptoms) that, when entered into WellDoc’s software, allows algorithms to help a patient adhere to a customized treatment plan that is as unique to the patient as his or her fingerprints. It’s a two-way information street. Doctors are empowered to more easily make the right therapy adjustments and patients can be supported each day via real-time and longitudinal feedback to enhance their self-management and follow their treatment plans. As a result, a patient never has to be “alone” anymore. Clinical trials show that people with Type 2 diabetes who used WellDoc, along with their usual care, lowered their A1c levels by more than a full point, significantly more than patients whose treatment plan did not include WellDoc. At this point, WellDoc is the only company with an FDA-cleared Mobile Integrated Therapy for real-time patient coaching and clinical decision support for diabetes management.
“I really believe this [WellDoc] program saved my life. My A1c was 11.6% and now is 7.4%. I know I have more to go, but I finally feel like I can do it.” — Sharon P., Clinical Trial Patient, Baltimore, MD
Giving primary care physicians better tools to help their patients with diabetes is a very important aspect of both Telcare’s and Well-Doc’s systems. The ratio of endocrinologists and certified diabetes educators to people with diabetes is 100 to 1, and people are developing diabetes much faster than the medical profession turns out new specialists. Three out of four new cases of diabetes are diagnosed by PCPs, and they remain the primary caregivers in a majority of cases.
Entrepreneurial enterprises aren’t the only ones who see opportunity in mobile health. The very biggest medical equipment and pharmaceutical companies, such as Johnson & Johnson and Sanofi, also have joined the chase.
Verio IQ – Automated Pattern Alerts
The J&J OneTouch entry is a new smart glucometer, the OneTouch Verio IQ (www.onetouch.com/verio). The device collects and stores glucose readings just like other meters, but with a twist: an option for on-screen pattern alerts. A typical on-screen message might read, “Looks like your glucose has been running low around this time.” If you want details, the next screen shows the actual readings and times of day they occurred. OneTouch Verio IQ comes with pre-set before-meal high limits of 130 mg/dl and before-meal low limits of 70 mg/dl, but these can be adjusted. Two low readings within the same 3-hour window) in a 5-day period produce a warning; it takes 3 before-meal high readings in the same 3-hour window over 5 days to trigger a “high” message. A handy companion printed guide is available that gives you possible causes and potential actions related to lows or highs. The guide fits in the meter case and organizes information around four different parts of day, from “before breakfast” to “after dinner/ overnight.”
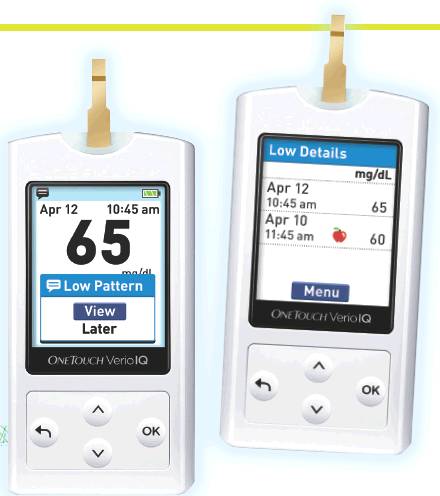 Verio IQ: Pattern recognition without logbooks!
Verio IQ: Pattern recognition without logbooks!
Kamal Bhandal, a Lifescan spokesperson for the product, explains the benefits as follows: “OneTouch VerioIQ is a fantastic meter for all people with diabetes — it makes testing simple. Many people with diabetes manage in the moment, correcting high or low blood glucose based on a single meter reading. Looking at your glucose patterns is a much better way, because it allows you to match your numbers to your actions.”
The importance of patterns in blood glucose test results and what they can tell either the patient or the caregiver about lifestyle impact and possible courses of action is well documented. Unfortunately, previous advances in meter technology that allowed people to upload their results into a PC or App-based storage and mapping utility appear to have been most useful to and most used by — you guessed it — the same people who bothered to keep ink-on-paper logbooks. Technology advances weren’t increasing adherence among patients who could probably benefit from it the most.
There is clearly a dual impetus behind Verio IQ’s launch. First is the product’s appearance. It looks much more like a smartphone (can anyone say “Apple”?) than a “traditional” glucose meter, most of which look suspiciously like, well, old cell phones. The second is more important than appearance, and aims directly at the very large number of people with diabetes who have read about pattern management and the virtues of keeping a logbook or uploading the data into a PC forever, but haven’t taken the time to do the work. “If you can’t be bothered,” Verio seems to say, “we’ll do the work for you.” It’s a perfect example of masking the complexity of technology to just deliver a result that the user needs to make intelligent decisions or accomplish a task. This, of course, was the core element of the late Steve Jobs’ genius.
iBGStar – The Future of Glucometers?
iPhone, iPod and iPad envy are pervasive in all technology companies, and medical device makers are no exception. Perhaps it’s a bit ironic, then, that one of the most innovative new glucometers was created, not by an established equipment maker, but by a pharmaceutical company entering the device market for the first time. Sanofi’s iBGStar (http://www.ibgstar.us/) entered the European market in April 2011, and became available in the U.S. about a year later, in May 2012. Its introduction makes Sanofi the first diabetes-focused company with a complete line of insulin-based products, including Lantus, Apidra, insulin pens, and a glucometer.
Designed to plug into the power port on an iPhone or iPod Touch, the iBGStar is a bit more than 2 inches long and less than an inch high. It is the first iPhone-enabled glucose meter to receive FDA approval and is sold in Apple’s retail stores, along with other health care devices like a WiFi-enabled scale and a blood pressure monitor dock. Apple stores seem to sprinkle anything they sell with pixie dust; the very fact that iBGStar is sold there automatically makes it cool. As one PWD put it, “Seeing it in the Apple Store made me think that diabetes is mainstream for the first time.” iBGStar can be used alone or plugged into an iPhone or iPod Touch. Either way, it syncs with the free iBGStar Diabetes Manager App and allows users to view their data, including test results — carbohydrate intake, and insulin doses — over time. Scorecards show individual blood glucose results and are color coded so that high and low blood glucose results can be more easily identified. Trend charts give users customizable views of their results and allow them to see whether values are within a defined target range. Anything the App compiles can be sent to someone as an email. Perhaps it’s worth noting that more than half of all physicians in the U.S. own an iPad. It’s fair to assume that where there’s an iPad, there’s probably an iPhone, so a lot of the advice-givers are ready to be linked.
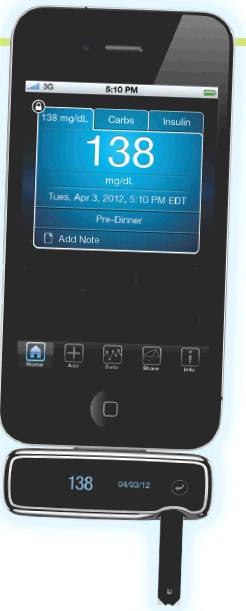 Like all things Apple, a very cool tool
Like all things Apple, a very cool tool
Are smartphone plugins the future of glucose measurement and diabetes management? Apple won’t comment on this line of speculation, but it will not be a surprise to see others following Sanofi’s lead. Perhaps one day we’ll even see a marriage of these connected devices to the intelligence of automated patient coaching and clinical decision support such as that offered by WellDoc , across all cellular and glucose measurement platforms.
The four examples cited here are not the only attempts to bring diabetes management into the 21st century. Technology’s ability to connect and empower continues to expand at breakneck speed, and is not the barrier to widespread connectivity between and among both patients and caregivers. Instead, it’s the health care system itself that gets in the way. Diabetes could be a test case for a new model of health maintenance and patient empowerment. It’s high time to begin, before the disease collapses the existing system and millions of people die prematurely and needlessly.
Thanks for reading this Insulin Nation article. Want more Type 1 news? Subscribe here.
Have Type 2 diabetes or know someone who does? Try Type 2 Nation, our sister publication.